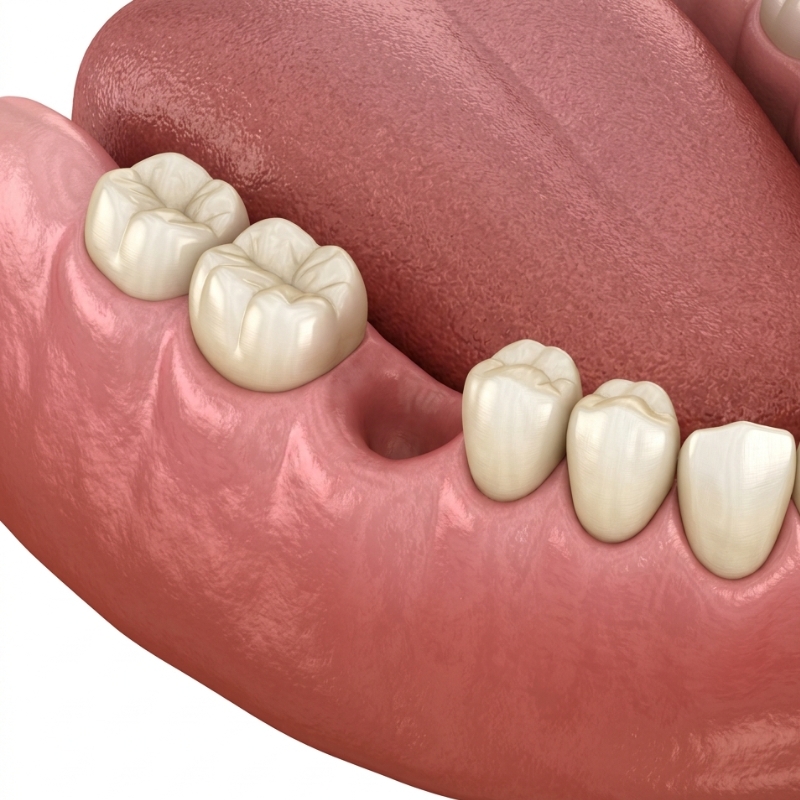
A missing tooth can feel surprisingly easy to ignore at first, especially if it’s a back tooth that doesn’t show in photos. But your mouth is a “team sport”: every tooth helps stabilise the bite, guide chewing, protect the jaw joint, and keep bone healthy—and that’s why options like dental Implants are often discussed when one tooth disappears and the rest of the system starts adapting.
Sometimes those adaptations are minor. Other times, they quietly snowball into shifting teeth, gum issues, a changed bite, and ongoing strain that’s harder (and more complex) to manage later.
This guide breaks down what can happen if you don’t replace a missing tooth, why bone changes occur, how your bite can drift, what symptoms to watch for, and what you can do right now to protect the area while you decide on your next steps.
Why a missing tooth can cause more than a gap
When a tooth is present, it does three important jobs that you don’t usually think about:
• It transfers chewing forces into the jawbone, which helps maintain bone volume
• It keeps neighbouring teeth in position, like a bookend on a shelf
• It meets an opposing tooth, keeping both teeth stable in the bite
Remove one piece and the “balance” changes. Your mouth is good at compensating, but compensation isn’t always harmless.
The three big changes that often follow
- Bone changes in the jaw where the tooth used to be
- Tooth movement (nearby teeth drifting or tilting into the space)
- Bite problems (including the opposing tooth moving and the bite becoming uneven)
The speed and severity vary depending on:
• Where the missing tooth is (front vs back, upper vs lower)
• Whether it’s a single tooth or multiple teeth
• Your gum health and bite pattern
• Whether the tooth was missing due to trauma, decay, or gum disease
• Habits like clenching/grinding (common during stress)
Bone changes: why the jawbone can shrink after tooth loss
Your jawbone isn’t static. It’s living tissue that remodels based on use. When a tooth is removed, the bone in that area loses a key source of stimulation: chewing forces transmitted through the tooth root. Over time, the body may resorb (break down) bone that it no longer “needs” to support a tooth.
What bone loss can look like in real life
Bone changes can be invisible at first, but they may show up as:
• A “dip” in the gum ridge where the tooth used to be
• A changed gum line or a darker triangle near the gap
• Less support for the lip or cheek in that spot (more noticeable with front teeth or multiple missing teeth)
• A feeling that food traps more easily because the gum contour has changed
Bone remodelling can begin relatively soon after extraction, but it’s not the same for everyone. Some people notice very little; others see faster changes, especially if gum disease contributed to tooth loss.
Quick answer
If a tooth is truly missing (root and crown), the bone that used to support it often reduces over time to some degree. The key point is that bone changes are generally localised to the area of the missing tooth, but local changes can still influence neighbouring teeth and the bite.
If you’re weighing long-term options, it can help to understand how bone behaves because it may affect what’s feasible later. If you want background reading on tooth replacement approaches, the Australian Dental Association has a patient overview you can browse here: Australian Dental Association information on dental implants.
Teeth shifting: why the gap rarely stays the same
Teeth naturally drift throughout life (even without braces history). When a tooth is missing, the teeth next to the gap can start leaning into the space. This can create new angles and ledges that trap food and plaque.
Common movement patterns include:
• The tooth behind the gap tipping forward
• The tooth in front drifting backwards
• Rotations (a tooth subtly turning)
• The contact points between teeth changing, which affects flossing
Why tooth movement matters (it’s not only cosmetic)
Shifted teeth can lead to:
• Harder cleaning (new “food shelf” areas)
• Increased risk of decay on exposed sides of teeth
• Gum irritation or inflammation around awkward contact points
• Bite imbalance that increases wear on specific teeth
• A feeling that your teeth “don’t fit together” like they used to
Even if you can’t see the movement day-to-day, your mouth adapts. You may start chewing more on one side without realising it, which can create its own pattern of wear and strain.
Q&A: How long can you leave a missing tooth before problems start?
There isn’t a universal countdown clock. Some people experience noticeable movement sooner; for others it’s subtle and slow. Where the tooth is missing and how your bite loads the area matters a lot.
A practical way to think about it:
• If you’re already noticing food packing, a change in how floss slides, or a new gap opening elsewhere, movement may already be happening.
• If you’ve had orthodontic treatment in the past, teeth can be more inclined to drift without stabilising contacts.
Bite problems: what “bite change” actually means
Your “bite” (occlusion) is the way your upper and lower teeth meet. It’s not a single snap-together point; it’s a complex set of contacts that guide chewing and jaw movement.
When a tooth is missing, two bite issues become more likely:
• Neighbouring teeth shifting changes the bite line
• The opposing tooth can over-erupt (move further down or up into the gap)
Over-eruption: the sneaky change many people don’t expect
If you lose a lower molar, for example, the upper molar that used to bite against it may slowly creep down into the empty space. The opposite can happen if an upper tooth is missing.
Over-eruption can:
• Create a “high spot” that hits first when you bite
• Make the bite feel uneven or “tilted”
• Increase chipping risk on the over-erupted tooth
• Make later replacement planning more complicated (because there’s less room)
Signs your bite may be changing
You might notice:
• You hit one side first when you close your teeth
• Chewing feels awkward or less efficient
• You’re avoiding the gap side without thinking
• New sensitivity or wear on a specific tooth
• Jaw fatigue after eating, especially chewy foods
• Tension headaches that seem linked to clenching
Not every headache is dental, but bite imbalance and clenching can be contributing factors for some people.
Q&A: Can a missing tooth cause jaw pain?
It can contribute. When you chew unevenly or your bite changes, muscles may work harder on one side, and the jaw joint can be loaded differently. If you already clench or grind, the imbalance can be more noticeable.
If you develop jaw locking, sharp joint pain, or persistent headaches, it’s worth getting checked sooner rather than later so you can rule out other causes and avoid compounding strain.
The “hidden” risks: cleaning problems, gum irritation, and a higher maintenance mouth
A gap changes how food moves across your teeth. It’s common to feel:
• More food trapping where the missing tooth used to be
• Gum tenderness from repeated packing
• Bad breath from trapped debris
• A feeling that brushing “doesn’t reach” properly
This can set up a cycle:
• Food trapping increases inflammation
• Inflamed gums are more likely to bleed and harbour bacteria
• Gum irritation can affect the teeth next to the gap
• Neighbouring teeth may become more vulnerable over time
If gum disease contributed to the missing tooth in the first place, leaving the gap untreated can sometimes make it harder to keep the entire area stable.
Front tooth vs back tooth: does the location change the risk?
Yes.
If it’s a front tooth
Concerns often include:
• Speech changes (air flow differences can cause a slight lisp)
• Confidence in social and work situations
• Gum contour changes that become visible
• Greater noticeability of drifting
If it’s a back tooth
Concerns often include:
• Chewing efficiency (you may avoid that side)
• Increased load on remaining molars (more wear or cracks over time)
• Over-eruption of the opposing tooth
• “Silent” bite drift you don’t notice until it feels off
A missing molar that you “can’t see” can still be a big deal because molars do most of the heavy lifting during chewing.
A simple self-check you can do at home
You can’t diagnose yourself, but you can monitor changes. Try this once a month:
• Look: In the mirror, compare the gum ridge on each side. Is the gap area flattening or dipping?
• Floss: Does floss now snag or slide differently around the teeth beside the gap?
• Bite: Gently close your teeth and notice if one side contacts first.
• Chew: Are you unconsciously chewing mostly on one side?
• Food trap: Are you consistently picking food out of the same spot?
If you notice a trend, it’s a sign to get the area assessed—especially if it’s paired with sensitivity, bleeding gums, or bite discomfort.
What you can do now if you’re not ready to replace the tooth yet
Sometimes timing matters—budget, health, family commitments, or anxiety can delay decisions. If you’re in a “not yet” phase, focus on preventing the gap area from becoming a bigger problem.
Daily care strategies
• Brush gently along the gum ridge where the tooth was, not just the neighbouring teeth
• Use interdental brushes if flossing is awkward (pick a size that doesn’t force or injure the gums)
• Rinse after meals if food packing is frequent
• Keep up regular cleans—plaque around tilted teeth is harder to remove at home
If you want a clearer picture of what long-term fixed replacement can involve, it may help to learn more about dental implant treatment so you understand the general steps and aftercare expectations.
Eating strategies (without overloading one side)
• Try to distribute chewing rather than favouring the non-gap side
• Cut tougher foods smaller to reduce chewing force
• If you clench, be mindful during stress (many people clench while driving or working)
Q&A: If I wait, will it be harder to replace later?
Potentially, yes—mainly because space and bone can change. Teeth drifting or the opposing tooth over-erupting can reduce room. Bone changes can also influence what’s involved. That doesn’t mean “too late”, but it can mean the plan becomes more complex.
Common scenarios (and what they often mean)
“It’s been years and I’m fine”
You may be coping well—and that’s great. But “fine” can sometimes mean:
• You’ve adapted your chewing pattern
• Movement happened gradually so you didn’t notice
• The jaw joint and muscles have compensated quietly
If you’ve had the gap for years, it’s still worth checking the stability of the neighbouring teeth and the opposing tooth position, especially if you’ve recently noticed wear, sensitivity, or a changing bite.
“Food always gets stuck there now”
This often suggests a change in contact points, gum contour, or a tilted tooth edge, creating a trap. It’s a common early sign that the area’s maintenance needs have increased.
“My bite feels higher on one side”
A “high spot” sensation can come from tooth movement, over-eruption of the opposing tooth, or changes in how you’re closing your jaw. It’s worth assessing because persistent high contact can accelerate wear or cracking.
When you should book an assessment sooner
Because this article is informational, think of these as “don’t ignore” signs:
• Increasing pain, swelling, or a bad taste (possible infection)
• Bite feels noticeably different week-to-week
• A tooth beside the gap becomes sensitive or loose
• Bleeding gums around the gap area that doesn’t settle with good cleaning
• Jaw pain, clicking with discomfort, or locking
• Repeated food packing causing gum soreness
If any of these are present, early advice can prevent bigger problems—regardless of what replacement option you ultimately choose.
Understanding replacement choices without the sales talk
People replace missing teeth for different reasons:
• Chewing function
• Bite stability
• Comfort and confidence
• Protecting neighbouring teeth from overload or decay risk
If you’re exploring fixed options, you’ll often see the term “implants” used as shorthand, but the more useful question is what suits your bite, bone, gum health, and medical history. For readers comparing pathways, here’s a deeper explainer on dental implants for missing tooth replacement that may help you understand how they’re used and what they support.
FAQ
Does leaving one missing tooth untreated really matter?
It can. Even a single missing tooth can set off bone changes, tooth drifting, and bite adjustments—especially if it’s a molar that takes heavy chewing forces.
Will my jawbone shrink if I don’t replace the tooth?
Often, some reduction in the bone in that area occurs over time because the bone no longer receives stimulation through the tooth root. The amount varies.
Can the tooth above (or below) move into the gap?
Yes. The opposing tooth can over-erupt into the empty space, which may create a high spot and reduce room later.
Why do my teeth feel like they’re moving?
Neighbouring teeth may be drifting or tipping into the gap. You may notice changes in flossing, food trapping, or how your bite closes.
Can a missing tooth affect speech?
Front tooth gaps are more likely to affect airflow and cause slight speech changes. Many people adapt, but some notice a lisp or difficulty with certain sounds.
What if I’m missing a back tooth and it doesn’t bother me?
Back teeth still matter for chewing and bite stability. A “quiet” gap can still contribute to shifting and over-eruption over time.
What’s the best way to keep the area clean?
Brush along the gum ridge and clean between the teeth next to the gap carefully. Interdental brushes can help if flossing is awkward. Regular professional cleans can be useful because plaque builds more easily around tilted teeth.
If I grind my teeth, does a missing tooth make it worse?
It can increase uneven loading and wear because your bite is already under higher forces. If you suspect grinding, it’s worth discussing protective strategies.
If I’m exploring long-term fixed options, how do I look after them?
Any replacement option comes with maintenance, and good habits matter. If you’re researching ongoing hygiene and check-up rhythms, this guide to dental implant care in Sydney is a useful starting point.